 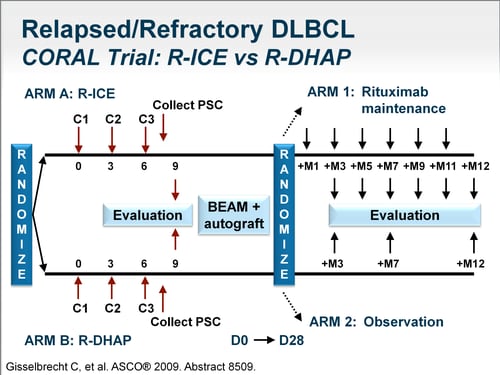
In an as treated analysis the difference between the RT and the no-RT arm was not significant (p = 0.136). 78% p = 0.007), mostly due to events caused by initiation of RT (n = 5) in the no-RT arm. 3-year EFS was superior in pts assigned to RT (94% vs. Response RT vs no-RT were CR/Cru 94% vs 84%, PR 2% vs 10%, PD 2% vs 4%. 96% (79/82) received RT per protocol and 5 pts in the no-RT arm received unplanned RT (4 after PR and 1 after CR/CRu). Results: 131 PMBCLs were included with a median age of 34 years, 54% were female, 79% had elevated LDH > UNV and 24% had E. Response was evaluated by the Internat Standardized Response Criteria, Cheson 1999. 
Primary endpoint was event-free survival (EFS), secondary endpoints were progression-free (PFS) and overall survival (OS). Pts were randomized in a 2 x 2 factorial design to 6xR-CHOP-14 or 6x-R-CHOP-21 without RT or with RT (39.6 Gy) to Bulk and E. Methods: The UNFOLDER trial included 18-60 year-old pts (aaIPI = 0 with Bulk or aaIPI = 1) qualifying for radiotherapy to Bulk or extralymphatic involvement (E). Therapy is based on R-CHOP or similar regimens, but the role of treatment intensification and consolidative radiotherapy (RT) is controversial, because data from randomized trials are rare. Background: Primary mediastinal B-cell lymphoma (PMBCL) is a distinct entity of aggressive lymphoma, which typically presents in young patients (pts) with a bulky mediastinal mass. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
